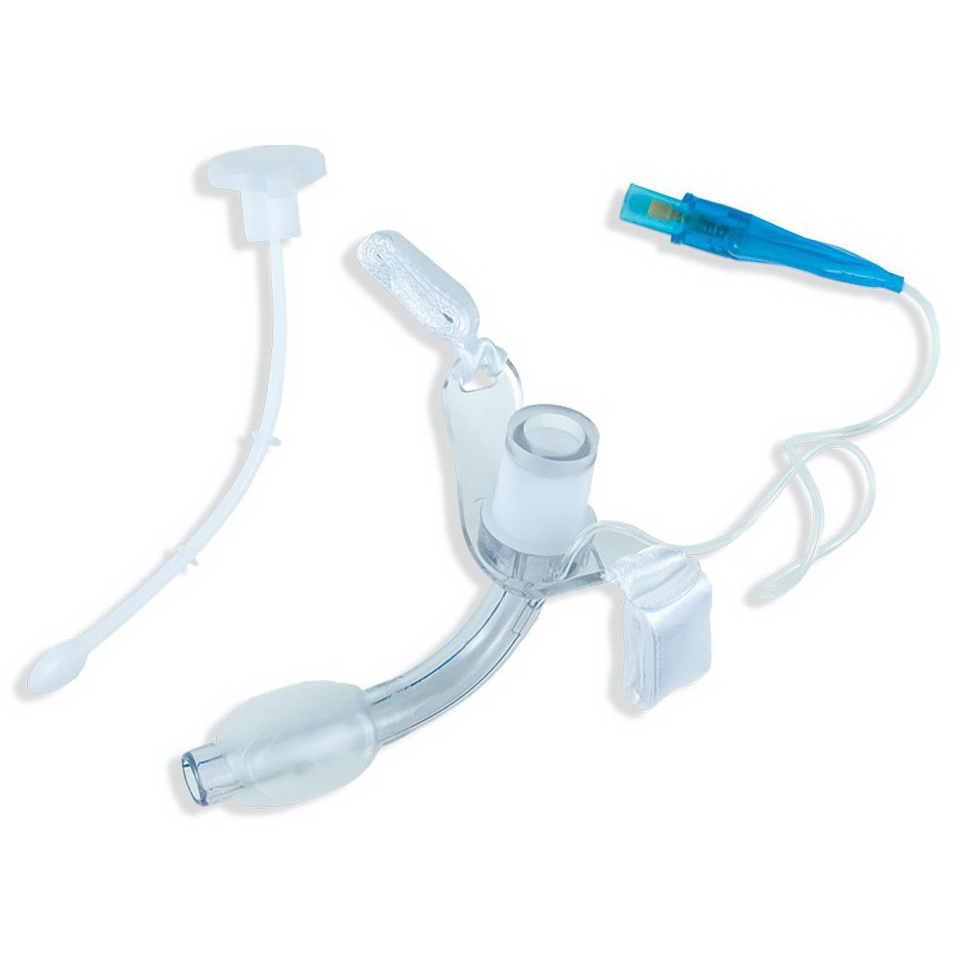
Cuffed tracheostomy tubes are only used for one reason: ensuring adequate oxygenation for patients who use mechanical ventilators. While the devices are not used to treat swallowing problems, it is not uncommon for patients who need cuffed tracheostomy tubes to suffer from dysphagia as well. This article will offer some insight into the relationship between tracheostomy tubes and swallowing disorders.
Heightened Risk of Aspiration
Patients with mechanical ventilation applied through cuffed tracheostomy tubes are at a much higher risk of aspiration, which occurs when food or liquids enter the lungs. Avoiding aspiration generally requires making dietary adjustments. Caregivers for tracheostomised patients may be interested in Simply Thick, a thickening agent designed to make liquids easier to swallow without adversely affecting that liquid’s taste, texture, or bioavailability.
Experts estimate that more than eight out of every ten patients with cuffed tracheostomy tubes also have problems with aspiration when they take food orally. To make matters even worse, aspiration doesn’t always trigger symptoms like coughing and throat clearing in patients with tracheostomy tubes, making it more challenging to identify potential risks.
When to See a Speech Therapist
Speech therapists often work with patients who have swallowing disorders to teach them safer ways to consume food orally. All tracheostomised patients who have experienced neurological problems should be referred to speech therapists before attempting to consume food, as should any patients who have undergone head or neck surgery. Patients who have already begun to consume food orally should be referred to a speech therapist for an evaluation if they show signs of aspiration, such as coughing, experience oxygen desaturation when they eat, or have anxiety about eating and drinking.
Treatments for Dysphagia in Tracheostomised Patients
Patients with extreme swallowing difficulties may need to be fed using alternative nutrition and hydration, but more often than not, patients are able to consume foods by mouth following speech therapy. Therapy typically involves focusing on abnormal swallowing behaviors. Patients may learn range-of-motion exercises to strengthen their muscles or alternative swallowing maneuvers such as increasing tongue base retraction and altered postural techniques like the head tilt or Mendelsohn’s maneuver.
Most patients will also have to switch to thickened liquids. Thin liquids like water, juice, and milk are more likely to enter the airway during swallowing, leaving patients at higher risk of aspiration. Thickening agents can be added to these liquids to make them safer to swallow.
The Importance of Oral Food Intake
Re-learning how to swallow safely and making changes to patients’ diets may be frustrating, but experts agree that, for the majority of patients, it’s the best solution. Alternative nutrition and hydration come with a lot of potential risks and side effects and, often, patients are unable to absorb as many nutrients as they would when consuming actual food on a dysphagia diet.
The Bottom Line
Using a tracheostomy tube with mechanical ventilation can make life difficult. Even little things like swallowing food can feel like insurmountable problems, but they don’t have to be. With the help of a speech therapist, most tracheostomised patients are still able to eat altered diets of approved foods and thickened liquids. This makes it much easier for patients to receive the nutrition and hydration they need to remain otherwise healthy despite their tracheostomies, improving their quality of life and preventing potentially serious medical complications.