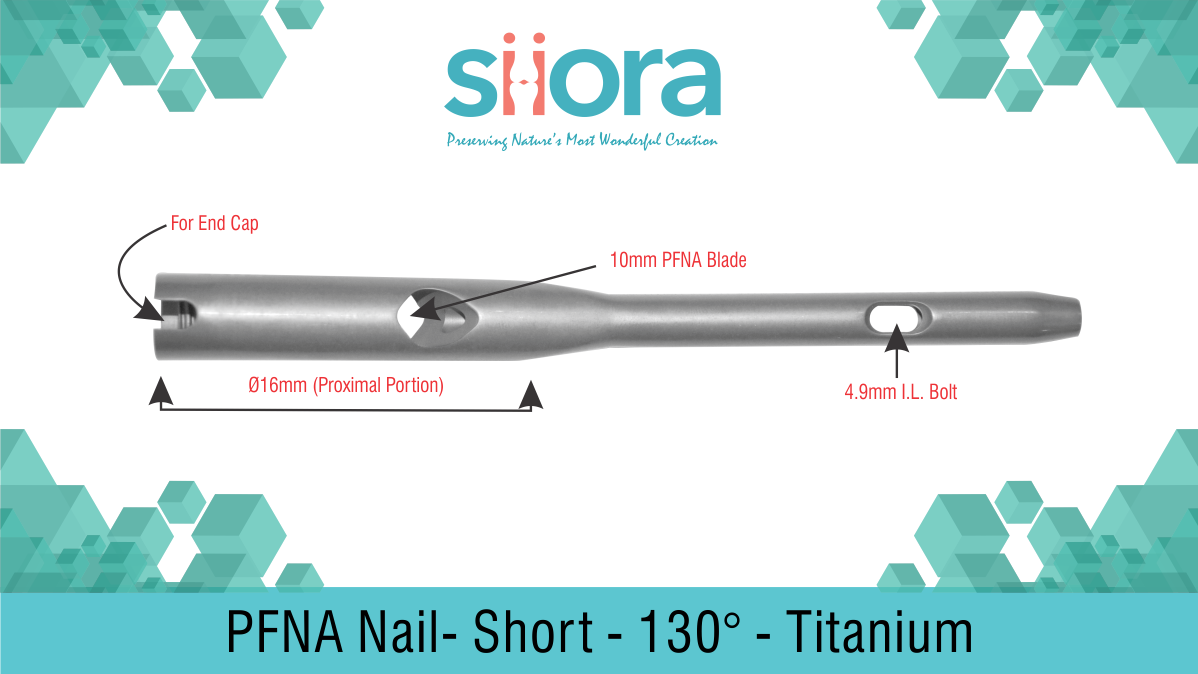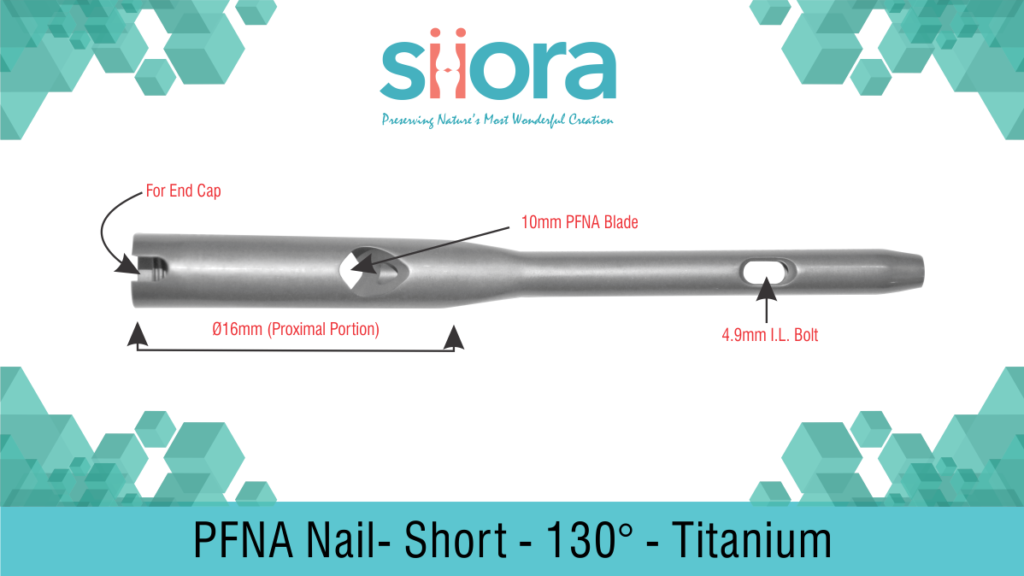
Normally, the common treatment of long bone shaft fractures is intramedullary nailing or inter-locking Proximal Femoral Nail Antirotation. Formerly, the application of the prevalent Kuntscher nail with its longitudinal slot was limited to midshaft diaphyseal fractures only. The main reason for its use was that the stabilization was based on the contact between the stiff bone and the elastic implant as per the concept of nailing. The area of contact between the bone and the nail is increased by the reaming of the medullary cavity thus it becomes suggestive of complex and distal fractures.
The mechanical features of the interface of the bone implant is also made better by permitting the use of the implants with a larger diameter. Though the reaming procedure has some intrinsic biological drawbacks specifically when it is carried out overly. These drawbacks are as follows:
- A noticeable increase in intramedullary pressure, the necrosis in the bone.
- The devitalization of cortical layers due to temperature rise.
Because of these drawbacks, the reamed nails’ use was restricted to the fractures in which only minor soft tissues were injured.
Universal Nails Locked and Tight Fitting
This nail was introduced by Grosse and Kempf. The interlocking nails were also added to this nail which significantly improves mechanical features of intramedullary implants. It also helped in enhancing the indication of more complex and distal fractures with an irregular pattern. Though the fixation in more distal or more complex fractures largely depends on the interlocking screws, not on the friction principle. Still the length of bone-implant design is functionally maintained as the locking screw restrains shortening. Though, the reduction in rotational stiffness is caused by the tubular nail’s longitudinal slot. It may lead to rotational instability. And it has specifically occurred in the case of nails with a smaller diameter.
Nailing Without Reaming Or Locking
Shaft fractures with critical soft-tissue injuries have been treated by using intramedullary nails by some groups in North America and Europe. These intramedullary nails were inserted unreamed so these were of loose-fitting. Rotational and longitudinal instability was the result because the implants like Ender nail, Rush pins and Lottes nail was too thin to lock distally or proximally particularly in a complex type of fractures. Although it had a low infection rate, yet the main drawback was the recurrent requirement of another undesired external stabilizer like plaster casts.
Nailing without reaming but with locking (Unreamed solid nail)
The noticeable requirement of a solid nail with a small diameter which could be locked was there. Even though the lack of a slot substantially increases the implant’s torsional stiffness, it also has the decreased capability to adjust to the shape of the bone. A correct fit can be a problem if the insertion location is not selected properly or if there is a divergence in the radius and shape of the intramedullary canal from that of the nail construct. The material solidity of the nail must be strengthened with a smaller outer diameter i.e. 9 mm in the femur to keep the possibility of implant failure as little as feasible.
The two requirements: low stiffness and high fatigue strength can be achieved by changing the material from stainless steel to the Ti- 6Al-7Nb, a titanium alloy. The use of larger locking bolts of 4.2/4.9 mm diameter (3.2/3.9 mm to start with)) is allowed by the higher strength of the nail. There are biological advantages of the firm cross-section of the nail but it does not contribute to its mechanical bending features. Many experiments on animals have been done. And the results show that infection susceptibility is less for the solid nail in comparison to the tubular nail with its internal dead space. On the contrary, the insertion of the nail in a cannulated or hollow system can be made easy and simpler by using a guidewire.