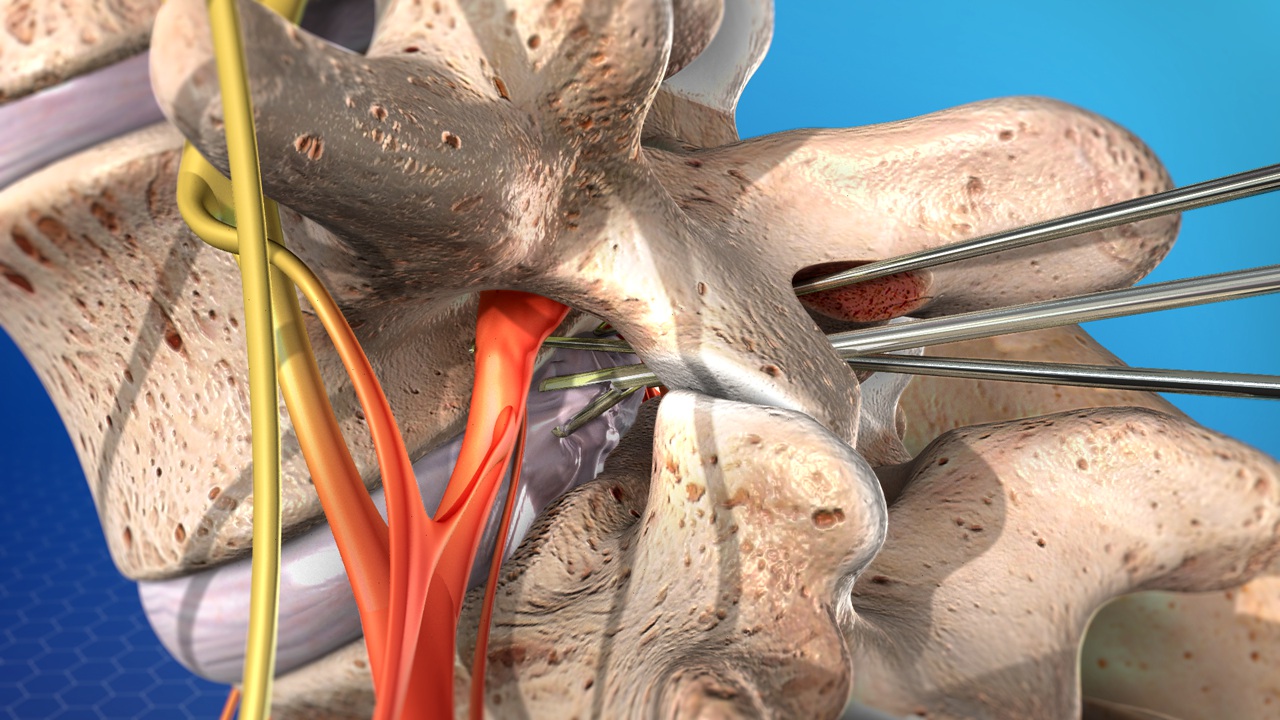
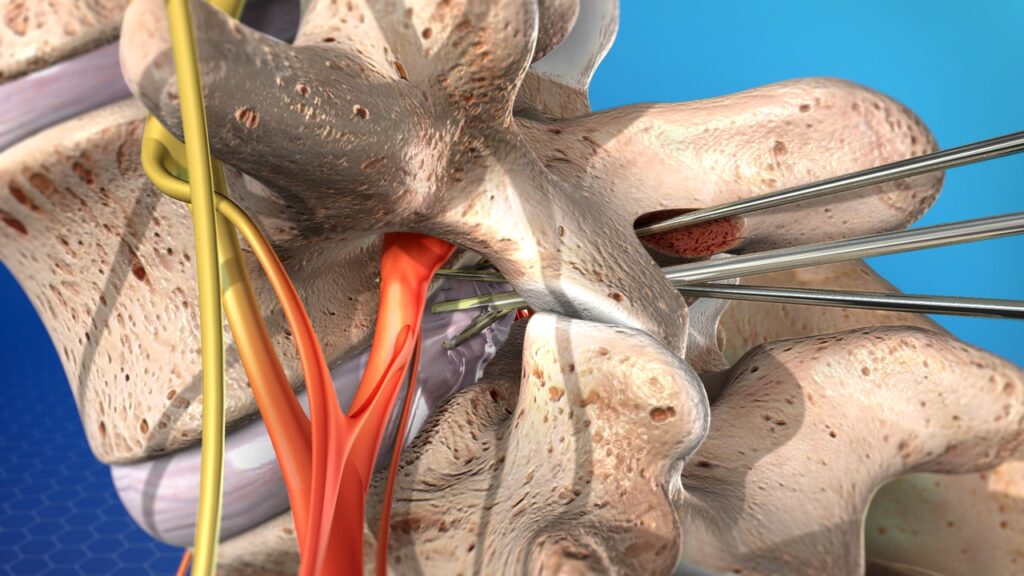
Microdiscectomy is not a new term in the medical space as the first successful operation was done in 1977. Techniques and equipment used in this procedure have been improving since then to give us the refined process that we have today. This minimally invasive surgery has proven essential in relieving pain.
However, there is still a portion of patients who are not sure about its effectiveness. You may be among those who want to know about its success rate, whether there are any risks associated with the procedure, and how long it takes to recover from the surgery.
Reasons to Perform a Microdiscectomy
Most people who go through this procedure have had nerve pain for a reasonable period. It is recommended for those who have tried other non-surgical approaches such as over-the-counter medications and physical therapy but still cannot overcome the pain.
This surgery can provide pain relief in the buttock area or pain that runs down on the legs. Ruptured disc patients seem to recover faster when they undergo surgery when compared to other approaches. However, patients in both surgical and non-surgical categories tend to have similar improvement rates after two to three years.
What is the success rate?
Research shows that microdiscectomy spine surgery has a success rate of 90% to 95%. However, the same report indicates the number of patients who are likely to develop recurrent disc herniation can be from 5% to 10%.
A recurrent disc herniation can reoccur just after the surgery, mostly within the first 3 months. It can also occur several years. A revision microdiscectomy is usually done after the reoccurrence. The success rate is the same during a reoccurrence. However, if there is another reoccurrence, the patient is exposed to 15 to 20% chances of reoccurrences.
A spine fusion surgery will come in handy if a patient multiple herniated disc recurrences. The doctor will remove the entire disc space and fuse the level to make sure that there are no recurrences. The recurrence is not mostly a result of the patient’s activity. The discs spaces have multiple fragments of discs that may come out later. The posterior microdiscectomy spine surgery will only remove about 5-7% of the disc space.
An artificial disc replacement can be done when the posterior joint is not compromised. Determining the best options when it comes to artificial disc replacement comes in handy to ensure that the patient gets a solution that fits his or her needs. The replacement removes the problematic disc and replaces it with an artificial one.
One should go through an exercise program of strengthening, stretching, and aerobic recondition of the back muscles after microdiscectomy spine surgery. The exercise program is also meant to eradicate pain and reduce the chances of recurrence.
How long does it take to recover?
A person who had undergone microdiscectomy surgery is expected to leave the hospital the same day or within 24 hours (unless there are complications). However, you can be referred to an occupational therapist to guide you on physical activities vital in the recovery journey.
The occupational therapist will guide you on how you should bend and twist your back after the surgery. Fully recovery from the procedure can take 2 to 3 weeks. However, you need to avoid engaging in extreme physical activities during this period.
Sitting for long hours will increase pressure on your back muscles and slow down the recovery process. Driving during the recovery period is also not advisable. The occupational therapist will highlight some of the activities that you should avoid during the recovery period.
Your home activities will not be affected much during the recovery period. However, the patient should take easy right after the surgery. Going up and down the stairs should not be a problem. Avoid lifting heavy objects, bending, and any other activity that will strain your muscles during this period. Do not forget to consult your physician if the pain persists even after the surgery.
Are there any dangers involved?
Any form of spine surgery has unique risks. Microdiscectomy spine surgery is no different and has the following risks:
Cerebrospinal fluid leak or dural tear
Only 1 to 2% of all surgeries done end with this complication. The risk does not affect the effectiveness of the procedure. However, the patient might be requested to lie flat for a day or two. This allows the leak to seal and also reduces the chances of suffering from a headache. Most of the patients with dural tear end up with headaches that go away after 24-48 hours. The dural tear does not come with any long term consequences.
Infection
The chances of suffering from an infection are very low. However, having a dirty operating table is the recipe for infections. They may occur several weeks and after the surgery and can be treated using IV antibiotics. The antibiotics can also be used during the surgery to reduce the chances of infection. An infection that spreads into the disc space may cause inflammation of the bone marrow.
Nerve Damage/Paralysis
It is very rare but can happen when the surgeon inadvertently cuts a nerve during the procedure. Some of the symptoms associated with nerve damage include weakness, pain and numbness. It is usually a temporal problem isolated to only one nerve. However, if it involves several nerves, then it can develop to be a permanent problem.
Who should avoid surgery?
If your pain is moderately tolerable or mild, then you shouldn’t opt for surgery. A typical surgery comes with loads of dangers, and you shouldn’t expose yourself to them when you are not much in pain. Other symptoms that may not require surgery include loss of a reflex, tingling, and numbness.
People that experience loss of muscle strength are not good patients for surgery. The muscles tend to regain strength on their own when they are treated through non-surgical approaches. Surgery can come in handy when the pain is found to be progressive or profound. Surgery is also essential when the patient loses bladder or bowel movement, even though it is rare.